My Quick Take | What Exosomes Are | Why Choose Exosomes | When Not Recommended | Patient Questions
My quick take
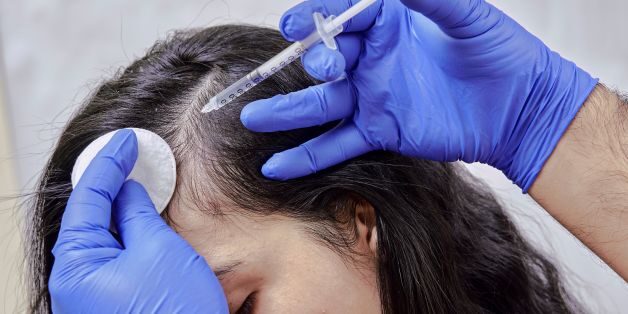
How exosome therapy helps with hair loss
When someone asks for exosome therapy for hair loss, I frame it as a regenerative adjunct. It may support selected patients when follicles are still present.
In my Mumbai practice, I consider exosomes mainly for:
- Early to moderate androgenetic alopecia (pattern hair loss), where miniaturised follicles still exist and the plan includes standard long-term care.[1][2]
- Patients with a sensitive, inflamed scalp, where calming the micro-environment is part of the goal.[3][4]
I aim for modest improvement, such as reduced excessive shedding and better hair calibre, over months.
What exosomes cannot do
I am careful about what exosomes cannot do, because in hair loss, false certainty causes the most harm.
- They do not reliably regrow hair in long-standing shiny bald areas where follicles are depleted.
- They do not “cure” androgenetic alopecia, which is chronic and needs maintenance.[1][2]
- They do not replace diagnosis. If the driver is iron deficiency, thyroid imbalance, postpartum shedding, crash dieting, traction, or scalp disease, we must address that first.[2]
Clear limits help patients choose wisely.
What exosomes are, in simple clinical terms
Exosomes are not stem cells
Exosomes are a type of extracellular vesicle, tiny particles released by cells that carry signalling molecules. In simple terms, they act like biological “messages” that can influence how nearby cells behave. In hair research, the interest is whether these messages can support follicle activity and reduce adverse inflammation.[3][4]
This is different from “stem cell therapy”. Many preparations are described as cell-derived, but are generally presented as cell-free products.
What is inside an exosome preparation?
Depending on source and processing, preparations may contain vesicles carrying proteins, lipids, and RNA that influence regeneration pathways.[3][4] The challenge is that “exosome” has become a broad label. The International Society for Extracellular Vesicles recommends clear characterisation and reporting standards (MISEV) because terms and methods can be inconsistent.[5]
Clinically, I use exosome treatments derived exclusively from vegetarian sources, ensuring safe, ethical, and highly effective results. Among these, Rose Exosomes, extracted from premium-quality rose cells, are at the forefront of my regenerative therapies, offering unparalleled benefits for skin and hair rejuvenation.
Why “exosomes” in cosmetics and “exosomes” in medical practice are often not the same conversation
Patients often come after seeing “exosome serums” online. Cosmetic use of the term can be loose. Medical discussions focus on extracellular vesicle preparations tied to early clinical data, with caution about what is proven.[3][4][5]
My practical advice is to separate:
- Cosmetic buzz, which is often vague.
- Medical hair-loss care, which must be diagnosis-led and monitored.
How exosome therapy is expected to work for hair
Follicle cycling basics, where exosomes may fit biologically
Hair follicles go through cycles of growth (anagen) and rest or shedding (telogen). In androgenetic alopecia, these follicles slowly shrink, leading to thinner hair and shorter growth phases over time.[1][2]
The idea is that extracellular vesicle signalling may help support the hair follicle environment and influence healthy hair growth cycles.[3][4][9]
Inflammation, micro-environment, and scalp health, the part patients underestimate
Many patients focus only on strands. Clinically, I also focus on scalp health. Dandruff-like inflammation, contact irritation, and folliculitis can keep shedding active and make people quit effective treatments early.
In Mumbai, humidity, pollution exposure, and styling can aggravate scalp sensitivity. If the scalp is inflamed, I stabilise it first, and consider exosomes only after.
How outcomes are judged in the clinic
When patients ask “Will I get new hair?”, I define response in practical terms:
- Shedding becomes less excessive over time, when shedding is trigger-driven.
- Hair calibre improves, hair looks a little fuller.
- Density improves mainly where follicles are miniaturised.
Because hair growth is slow, outcomes are judged over months.
Why choose exosomes as part of your hair plan
For male and female pattern hair loss
Indian expert consensus keeps medical options as the backbone for androgenetic alopecia, while procedures are adjuncts based on stage.[1]
I consider exosome treatment for hair in Mumbai when:
- The diagnosis is clear and early to moderate, with visible miniaturisation.[1][2]
- The patient wants an adjunct and understands that maintenance still matters.[1]
- We have addressed drivers like scalp inflammation, deficiencies, and damaging hair practices.
- My goal is to support the foundation, not replace it.
Post-transplant support
A transplant relocates follicles, it does not stop future miniaturisation of native hair. That is why long-term planning is important.[1][2]
I may consider regenerative adjuncts post-procedure for select patients, mainly to support scalp recovery and reduce inflammation. I do not support the idea that exosomes “replace” transplant planning or ongoing medical care.
Patients who have plateaued on other regenerative options
If someone has tried PRP or microneedling and feels stuck, I re-check basics before adding a newer procedure:
- Are we treating the right diagnosis, or is it mixed hair loss?
- Are triggers active, iron status, thyroid, crash diet, postpartum timing, stress?[2]
- Is scalp inflammation controlled?
- Is the maintenance plan realistic and consistent?
This review often improves outcomes more than switching procedures quickly.
When I do not recommend exosomes
Scarring alopecias and active inflammatory scalp disease
If I suspect scarring alopecia or active inflammatory scalp disease, my priority is diagnosis and medical control. A regenerative add-on is not first-line.
Completely slick areas, unrealistic density expectations
In long-standing shiny bald areas, follicles are often depleted. Exosomes are unlikely to recreate density, and I discuss other realistic options.
Uncontrolled triggers, thyroid, iron deficiency, crash dieting, high stress, postpartum timing
When shedding is driven by an active trigger, a procedure can become a distraction. Standard clinical discussions in hair loss emphasise ruling out and correcting contributors such as thyroid imbalance, iron deficiency, childbirth-related shedding, crash diet, and severe stress.[2]
If a key trigger is active and untreated, I do not start an advanced regenerative plan until we have addressed it.
Special situations, pregnancy, breastfeeding, autoimmune disease, immunosuppression
In pregnancy and breastfeeding, I generally avoid elective regenerative procedures due to limited safety data. In autoimmune disease or immunosuppression, I individualise and often take a conservative approach.
Personalising exosome therapy, how I combine it with other treatments
Back to hair loss basics
If I had to choose one message, it is this, foundations decide outcomes.
- Correct diagnosis and staging.[1][2]
- Scalp inflammation control.
- Evidence-based long-term therapy when appropriate, with honest counselling about maintenance.[1]
- Nutrition and lifestyle stabilisation when shedding triggers are present.[2]
Exosomes for hair growth, if used, should sit on top of this base.
Exosomes with PRP
PRP has a broader clinical evidence base in androgenetic alopecia than exosomes, including meta-analyses showing improvement in hair density in some patients.[6]
I combine only when there is a clear clinical reason and the patient understands that “stacking” does not automatically mean more benefit.
Exosomes with microneedling
Microneedling creates micro-channels in the scalp. Some clinicians combine this with topical exosome application, with the idea that delivery may be enhanced.[7][8] I use this combination selectively, for appropriate patients and stages.
Typical plans I use (early thinning, diffuse female thinning, post-transplant support)
These examples show my thinking, not rigid templates.
- Early male thinning, stabilise and maintain first, then add a regenerative adjunct if goals and stage match.[1][6]
- Diffuse female thinning, clarify triggers and deficiencies first, then consider adjuncts once the base is stable.[2]
- Post-transplant, protect native hair long term, consider adjuncts selectively for scalp recovery, not as a substitute for planning.[1]
When other treatments are prescribed instead
PRP, where it still makes sense
PRP is autologous and has a stronger evidence base in androgenetic alopecia than many newer regenerative options.[6] In selected patients it is a reasonable adjunct.
GFC and other growth-factor concentrates, where I place them
I place growth-factor concentrates as supportive adjuncts, similar in intent to PRP, used only when diagnosis is clear and follicles are still present. I keep expectations measured and focus on follow-up, because consistency matters more than novelty.
Hair transplant, when it becomes the right conversation
When density loss is advanced and medical options have been optimised, a hair transplant becomes the realistic conversation. A dermatologist’s job is to say this clearly, early.
What most people get wrong about exosomes for hair
“One session is enough”
Hair biology is slow, so outcomes are judged over months. I prefer structured follow-up and staged planning rather than assuming one session is a complete answer.
“It works even if the follicle is gone”
If follicles are depleted, signalling cannot recreate density reliably. This is why early intervention and realistic staging matter.
“It is the same everywhere, brand does not matter”
Extracellular vesicle preparations can vary based on source and processing. Scientific guidance exists because terminology and preparation can be inconsistent.[5] Brand matters only insofar as it reflects quality control and transparency. I opt for ASCE Rose Exosome from Korea.
“It is approved everywhere so it must be proven”
Trending does not mean proven. Even globally, regulators have acted against certain entities making unapproved drug-like claims for exosome products.[10] My advice is to ask what evidence exists for your type of hair loss and what safety controls are in place.
“If I shed after, it failed”
Shedding can fluctuate for many reasons, including ongoing triggers. This is why diagnosis, follow-up, and consistency matter more than one early signal.
Patient questions I often get
“How soon will I see less hair fall?”
Shedding patterns vary and depend heavily on the underlying cause. I set realistic expectations during consultation and plan follow-up accordingly.
“Can I combine it with my current hair loss medication?”
Combining with ongoing medical therapy is often part of the plan. I review what the patient is already using before recommending any add-on, because medical hair loss care is cumulative and must be coordinated.
“Is it safe for sensitive scalps?”
Preparations I use are from vegetarian sources and suitable for sensitive scalps. Timing is individualised. The goal is to protect the scalp barrier and avoid inflammation that can worsen shedding.
“Is it painful, and what numbing is typically used?”
Scalp procedures involve some discomfort, but tolerance varies. Numbing approaches can be used in clinical settings. Details depend on the patient and the clinician’s protocol, and should be discussed in person.
“How do I know the product is authentic and handled correctly?”
Ask for documentation on source, storage, and quality checks. Also ask whether the clinician can explain what the product is, rather than relying on vague “regenerative” language. Scientific standards exist because transparency protects patients.[5]
“Do I still need long-term maintenance if it works?”
For androgenetic alopecia, yes, some form of long-term management is usually needed because the tendency to miniaturise continues.[1][2] Exosomes may support, but they do not rewrite genetics.
References
- Mysore V, Shashikumar BM. Expert consensus on the management of Androgenetic Alopecia in India. Int J Trichology. 2019. URL https://pmc.ncbi.nlm.nih.gov/articles/PMC6580804/
- Kaliyadan F, Nambiar A. Androgenetic alopecia: An update. Indian J Dermatol Venereol Leprol. 2013. URL https://ijdvl.com/androgenetic-alopecia-an-update/
- Al Ameer MA, et al. Exosomes and Hair Regeneration: A Systematic Review of Clinical Evidence. 2025. URL https://pmc.ncbi.nlm.nih.gov/articles/PMC12433634/
- Gupta AK, et al. Systematic review of exosome treatment in hair restoration. J Cosmet Dermatol. 2023. URL https://pubmed.ncbi.nlm.nih.gov/37381168/
- Welsh JA, et al. Minimal information for studies of extracellular vesicles 2023 (MISEV2023). J Extracell Vesicles. 2024. URL https://pubmed.ncbi.nlm.nih.gov/38326288/
- Zhang XX, et al. Platelet-Rich Plasma for Androgenetic Alopecia: A Meta-analysis. Aesthetic Plast Surg. 2023. URL https://pubmed.ncbi.nlm.nih.gov/37533146/
- Dhurat R, et al. A Randomized Evaluator Blinded Study of Effect of Microneedling in Androgenetic Alopecia. Int J Trichology. 2013. URL https://pmc.ncbi.nlm.nih.gov/articles/PMC3746236/
- Jha AK, et al. Androgenetic alopecia and microneedling: Every needling should not be the same. J Am Acad Dermatol. 2019. URL https://www.jaad.org/article/S0190-9622%2819%2930460-8/fulltext
- Wu X, et al. Advances in the extracellular vesicles treatment of alopecia. Ann Med. 2025. URL https://www.tandfonline.com/doi/full/10.1080/07853890.2025.2543517
- U.S. Food and Drug Administration. New Life Medical Services, LLC, Warning Letter (includes exosome product references). 2025. URL https://www.fda.gov/inspections-compliance-enforcement-and-criminal-investigations/warning-letters/new-life-medical-services-llc-711102-09242025